Shaping a private provider sector that accelerates UHC: Foundational skills for public payers and policymakers
Countries pursuing universal health coverage (UHC) are increasingly active in seeking to leverage private healthcare providers to enhance their reforms. Many are contracting private providers to deliver subsidized care and/or corporatizing their public facilities in order to improve performance, tackle inefficiencies and stimulate much-needed new investment across the delivery systems. As most soon discover, this requires a very different set of skills to those traditionally developed among public healthcare officials, and a range of technical and cultural gaps become evident.
The Joint Learning Network on UHC (JLN) has already addressed some of these gaps through previous initiatives on communicating with and regulating private sector primary care providers. But there are so many more opportunities to share learning and build understanding between JLN member states – as well as between public and private institutions directly.
For this reason, a series of prioritization workshops was held to decide where the JLN should take its private sector focus next. Two topics stood out, both of which have now completed a foundational learning stage and produced a mini-guide which is released this week: contract management of private providers and harnessing private investment.
Contract management work stream
The first topic focused on contract management of private providers, described as the ‘Achilles Heel’ of many payers because, in the words of one participant: “all our focus seems to go into agreeing the contract, but afterwards we sit back”. Often treated as an administrative function, contract management can make or break a payer that relies heavily on private sector delivery. Weak contract management can lead to:
- Inability to determine whether money spent is producing results
- Insufficient levers to encourage (or force) providers to change
- Inability to detect and prevent fraud and gaming
- Conflict over the interpretation of contract terms
- A reactive, rather than proactive approach to problems that (inevitably) arise between payers and providers
Over three virtual workshops, participants from 13 JLN member countries worked through what contract management is, why it is important, what the enablers of success look like, and how one country – India – rose to the immense challenge of managing contracts for nearly 27,000 public and private providers under its AB-PMJAY coverage scheme.
Recognizing the many facets of good contract management, and the different ways that success could be defined, participants co-produced a framework to describe what an ‘ideal’ system of contract management would look like. They then used this tool to compare their current state against the ideal and identify priority actions for improvement based on the gaps.
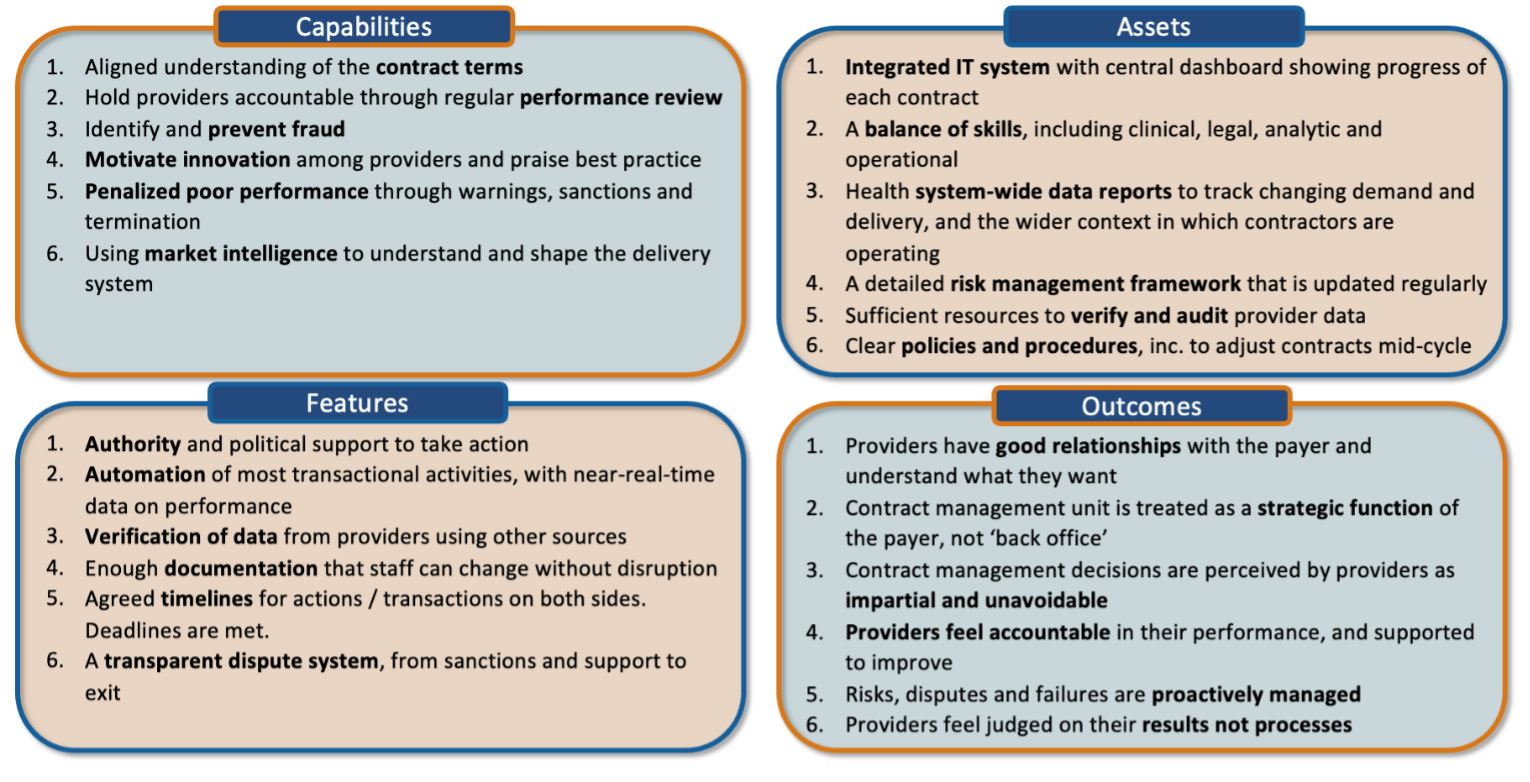
Private investment work stream
The second priority learning need was how to harness and direct private investment to enhance a government’s UHC agenda. Or, as one participant put it “we would like to partner more with the private sector, but what exists now just isn’t what we need”.
So how can public officials use the levers available to them to jump-state private investment into the kinds of services they would like to partner with, tapping into the more than US$200 trillion in capital markets globally to address the estimated US$200 billion annual gap in healthcare investment needed to achieve the health Sustainable Development Goals?
Properly harnessed, private capital can accelerate the pace of UHC reforms by creating new capabilities and capacity in the provider sector (especially where there are gaps) without drawing on public borrowing, as well as introducing new innovations and ways of working. Without government engagement, however, private investment can either be absent, or flow towards services that duplicate what already exists, do not meet the standards required by a payer, and draw resources (such as staff) away from universally-accessible services.
To improve understanding of these levers, over three virtual workshops participants heard from private investors and advisors about what private capital is, how it is deployed, how private investors evaluate a healthcare opportunity and what models of public-private partnership exist.
From these discussions a three-step process was co-produced for how governments can develop a strategy to strategically harness private investment. This starts with setting clear objectives as to where the private sector can make a unique contribution to the government’s UHC agenda and why, including how it could impede progress.
The next step is developing a supportive macro-level environment, tackling any barriers that exist beyond any individual project that the government might have in mind, for example whether the purchaser has a reputation for paying on time, whether data that investors will need to evaluate opportunities is being published, and ensuring a supportive banking, regulatory and tax system.
The third step is to focus on any project-specific partnerships that are a priority for government. The group discussed several different models running from simple infrastructure builds (noting that for a hospital the construction phase can be as little as five percent of the total lifetime cost of actually running it), to more complex concession and franchise models.
More detail is given on these steps in the mini-guide on private investment which is released this week, but the lessons were further illuminated through a case study from a former Minister of Health in Georgia about how it had sought to implement these lessons to renew its ageing provider infrastructure over the last 25 years.
What next?
Further stages of this work are planned for the future, including joint learning alongside private sector providers and investors to further build understanding and skills on both sides. In the meantime, both mini-guides are available now on the JLN website.
